Monitoring Your Clinic’s Medicare Compliance Within WebPT
It appears we have a theme going this week. Monday-Tuesday went over WebPT’s business reports. Yesterday was the ins and outs of the Plan of Care Report.

Subscribe
Get the latest news and tips directly in your inbox by subscribing to our monthly newsletter
It appears we have a theme going this week. Brooke devoted Monday and Tuesday to discussing WebPT’s business reports. Yesterday, I showed you the ins and outs of the Plan of Care Report. But monitoring your Medicare compliance doesn’t end there. Here are a few more helpful reports:
Medicare Payment Adjustment Report (MPAR)
The Medicare Payment Adjustment Report (MPAR) shows you how multiple procedure payment reductions (MPPR) are affecting your clinic’s profits and losses. Most practice management systems do not provide this data, so this report gives WebPT clinics a significant advantage as they can assess the impact of MPPR and adjust their processes accordingly.
To access the MPAR, click “MPA Report,” located under the Reports section on the left side of the WebPT application. Once inside the MPAR, you will see search fields for Time Period, Patient, and Therapist. You’ll create the report using the Patient field. Simply search for a Medicare patient with finalized notes. Patient names will start to appear as you type, but be sure to enter a minimum of three letters. To access a patient, select his or her name and click “Generate Report.”
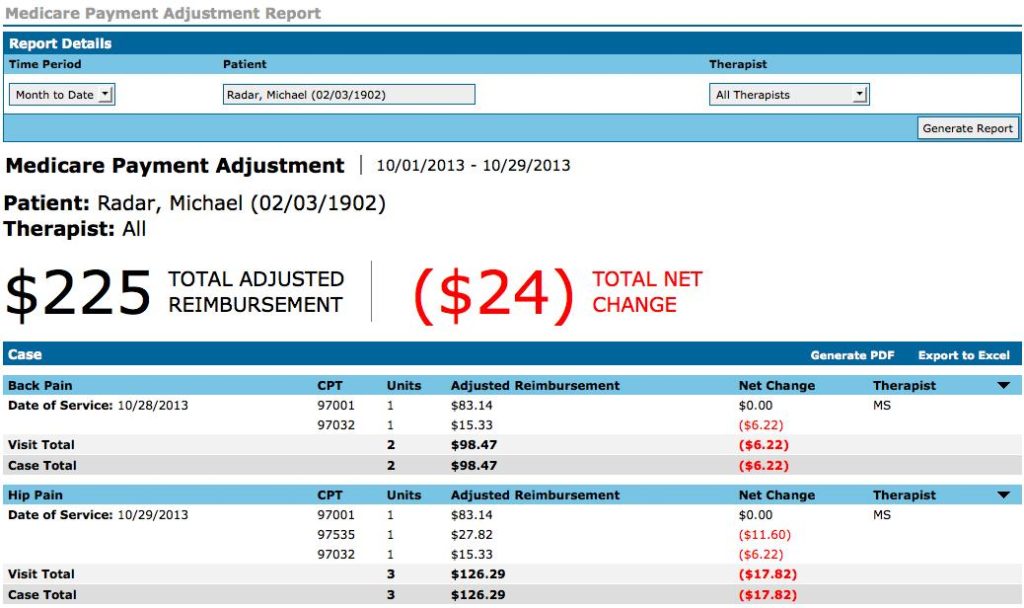
To see additional screenshots and further instructions, check out the MPAR user guide.
According to the Centers for Medicare & Medicaid Services (CMS), the MPPR-applied discount for institutional and noninstitutional facilities will be 50% on the second and subsequent procedure each day. You can view fee amounts inside the Medicare Fee Schedule (located in your clinic’s dropdown menu in the top-right corner of your WebPT dashboard). Please note that in order for the Medicare Fee Schedule to function, you must select regional location and facility type within Clinic Settings, which you can also access from your clinic’s dropdown. We pull these fees directly from CMS. For more on MPPR calculations and formulas, check out this CMS page and this APTA page.
For more details on MPPR and the fee schedule, check out this user guide.
Medicare Cap Report
Another essential compliance report is the Medicare Cap Report, which allows you to view your Medicare patients’ progress toward the therapy cap. It also enables you to see whether your therapists have attached the KX modifier for those patients who’ve exceeded the cap. This report also has an alert system associated with it. The rules of the therapy cap can be overwhelming and tricky, to say the least. Luckily, our report and alerts help keep you on the right side of the regulations.
To access the Medicare Allowable Cap Report, click “Medicare Cap Report” located under Reports on the left side of the Dashboard.
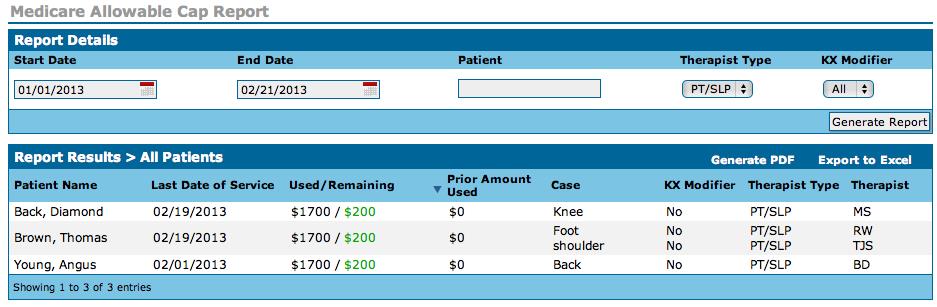
As for the alerts, they appear when a patient is:
- approaching the cap
- exceeding the cap (time to attach the KX modifier!)
- approaching the Manual Medical Review threshold ($3,700)
- exceeding the Manual Medical Review threshold (in which case you must apply to CMS for a manual medical review)

Another WebPT perk? For those who have the Front Office Package, you can view a patient’s progress toward the therapy cap within the Scheduler.
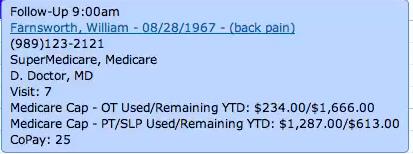
Click here to access the therapy cap report and alerts user guide.
FLR Report
Speaking of tricky Medicare regulations, functional limitation reporting (FLR) was probably the most intense Medicare regulatory change in all of 2013. Not only did WebPT create an integrated reporting tool to ensure you’re FLR compliant, but we also developed a report that provides you with real-time business intelligence regarding FLR. The report shows you:
- patients seen
- total visits
- G-codes reported, as well as those used most frequently
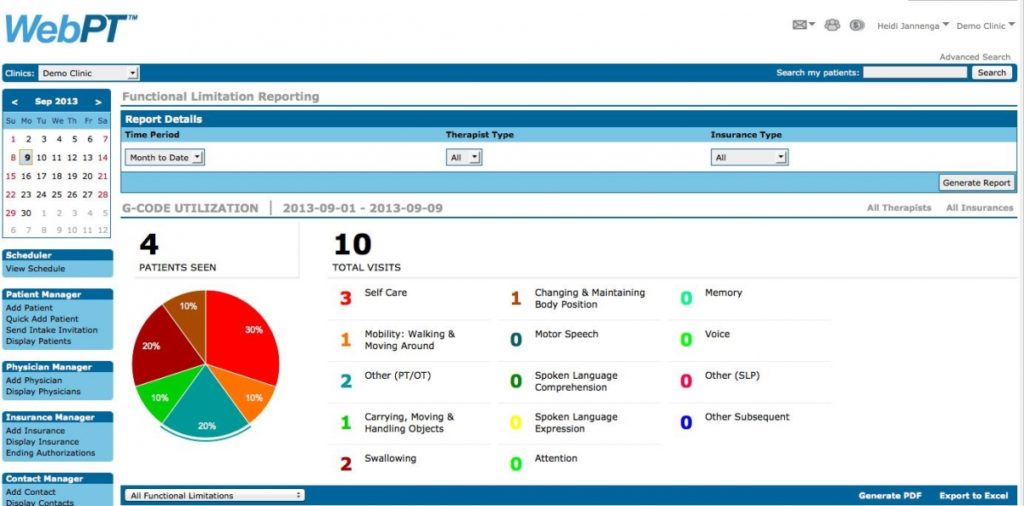
Under the Report Summary, you can also view live statistics organized by therapist. Using the dropdown menu, you can choose to display certain functional limitations. You can generate both the report and summary based on time periods, therapist types, or insurance types.
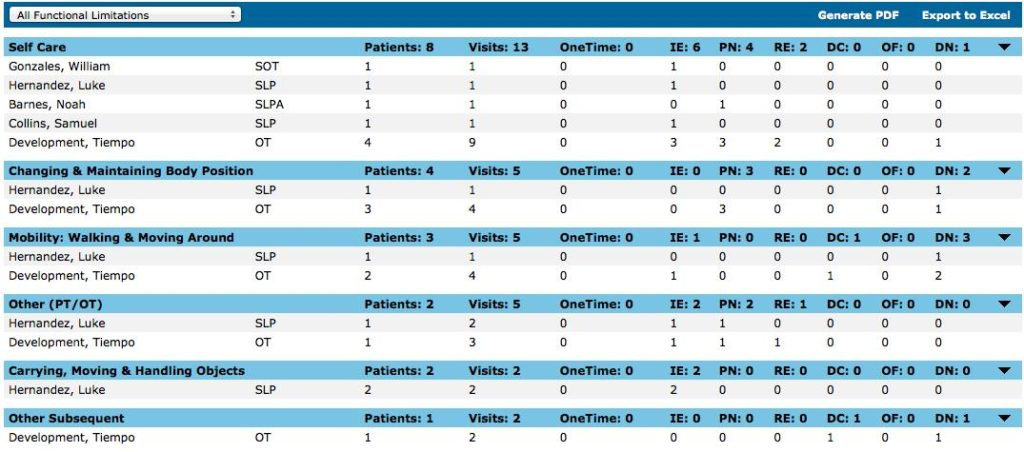
To learn more, check out the FLR report user guide.
WebPT is your partner in compliance. That’s why we’ve developed these reports—to ensure your clinic has all the resources necessary to monitor your Medicare compliance. Yes, these regulations can be frustrating, but with our reports, alerts, and tools, you can breathe easier. Have questions about these reports or compliance in general? Ask them in the comments section below.





